Hip Arthritis
What is Hip Arthritis?
The term arthritis literally means inflammation of a joint but is generally used to describe any condition in which there is damage to the cartilage. Inflammation is the body's natural response to injury. The warning signs that inflammation presents are redness, swelling, heat and pain.
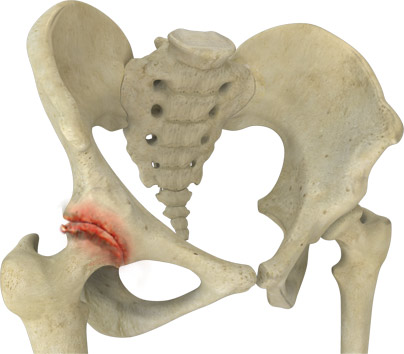
The cartilage is a padding that absorbs stress. The proportion of cartilage damage and synovial inflammation varies with the type and stage of arthritis. Usually, the pain early on is due to inflammation. In the later stages, when the cartilage is worn away, most of the pain comes from the mechanical friction of raw bones rubbing on each other.
Types of Hip Arthritis
There are over 100 different types of rheumatic diseases. The most common are:
Osteoarthritis: Osteoarthritis is also called as degenerative joint disease; this is the most common type of arthritis, which occurs often in older people. This disease affects cartilage, the tissue that cushions and protects the ends of bones in a joint. With osteoarthritis, the cartilage starts to wear away over time. In extreme cases, the cartilage can completely wear away, leaving nothing to protect the bones in the hip, causing bone-on-bone contact. Bones may also bulge, or stick out at the end of the hip, called bone spurs.
Osteoarthritis causes joint pain and can limit a person's normal range of motion (the ability to freely move and bend a joint). When severe, the hip may lose all movement, causing a person to become disabled.
Rheumatoid arthritis: This is an auto-immune disease in which the body's immune system (the body's way of fighting infection) attacks healthy joints, tissues and organs. Occurring most often in women of childbearing age (15-44), this disease inflames the lining (or synovium) of the hip. It can cause pain, stiffness, swelling, and loss of function in the hip. When severe, rheumatoid arthritis can deform or change the hip.
Rheumatoid arthritis tends to be symmetrical. This means the disease affects the same joints on both sides of the body at the same time and with the same symptoms. No other form of arthritis is symmetrical. About two to three times as many women as men have this disease.
Post-traumatic arthritis: Arthritis developing following an injury is called as post-traumatic arthritis. The condition may develop years after the trauma such as a fracture, severe sprain or ligament tears.
Psoriatic arthritis: This form of arthritis occurs in some persons with psoriasis, a scaling skin disorder.
Causes of arthritis
Osteoarthritis is caused by the wearing out of the cartilage covering the bone ends in the hip. This may be due to excessive strain over prolonged periods of time, or due to other diseases, injury or deformity. Primary, osteoarthritis is commonly associated with ageing and general degeneration of the hips.
Secondary osteoarthritis is generally the consequence of another disease or condition, such as repeated trauma or surgery to the hip, or abnormal joint structures from birth.
Rheumatoid arthritis is often caused when the genes responsible for the disease are triggered by infection or any environmental factors. With this trigger, the body produces antibodies, the defence mechanism of the body, against the hip and may cause rheumatoid arthritis.
Fractures at joint surfaces and joint dislocations may predispose an individual to develop post-traumatic arthritis. It is considered that your body secretes certain hormones following injury which may cause death of the cartilage cells.
Uric acid crystal build-up is the cause of gout and long-term crystal build-up in the joints may cause deformity.
Symptoms of Hip Arthritis
Symptoms vary according to the form of arthritis. Each form affects the body differently. Arthritic symptoms generally include swelling and pain or tenderness in one or more joints for more than two weeks, redness or heat in a joint, limitation of motion, early morning stiffness, and skin changes including rashes.
Diagnosis of Hip Arthritis
Doctors diagnose arthritis with a medical history, a physical exam and X-rays of the hip. Computed tomography (CT) scans and magnetic resonance imaging (MRI) scans are also performed to diagnose arthritis.
Treatment Options for Hip Arthritis
There is no cure for arthritis. Your doctor may prescribe anti-inflammatory medicine, occupational therapy or physiotherapy, which includes exercises and heat treatment. In severe cases, surgery may be suggested. The type of surgery will depend on your age and severity of the disease. In the elderly, with severe arthritis, hip joint replacement can give good results.
Initial treatment for arthritis is conservative, consisting of rest, avoidance of vigorous weight-bearing activities, and the use of non-narcotic analgesic and/or anti-inflammatory medications. With worsening of symptoms, a cane or braces may be helpful. For more severe symptoms, an injection of cortisone into the joint is frequently advised and can be quite helpful. When conservative measures have been exhausted, offer no relief, and have become disabling, surgery may be recommended. Surgery is usually considered if non-surgical treatment fails to give relief. There are different surgical procedures that can be performed and may include:
Synovectomy: This surgery is usually indicated for early cases of inflammatory arthritis, where there is significant swelling (synovitis) that is causing pain or is limiting the range of motion. Synovectomy is the surgical removal of the inflamed synovium (tissue lining the joint). The procedure may be performed using arthroscopy.
Arthroplasty: In this procedure, your surgeon removes the affected hip joint and replaces it with an artificial implant. It is usually performed when the hip is severely damaged by osteoarthritis, rheumatoid arthritis, post-traumatic arthritis or avascular necrosis. The goal of the surgery is to relieve pain and restore the normal functioning of the hip joint. Total hip joint replacement can be performed through an open or minimally invasive approach.
Arthrodesis: A fusion, also called an arthrodesis, involves removal of the joints and fusing the bones of the joint together using metal wires or screws. This surgery is usually indicated when the joints are severely damaged, when there is limited mobility, damage to the surrounding ligaments and tendons, failed previous arthroplasty, and when heavy manual use is expected.
Your surgeon will discuss the options and help you decide which type of surgery is the most appropriate for you.